Browse By Category
LATEST NEWS
OUR BLOG SPACE
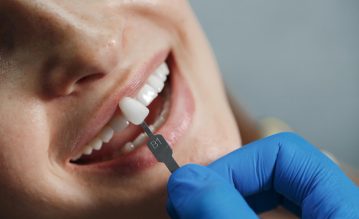
View AllWhy Retainer Material Selection Matters In Post-Orthodontic Care
Are all removable retainers the same? The answer is obviously no. Some are comfortable for the patient, look good, and last long enough to hold the results of orthodontic treatment in place. Others struggle to provide effective retention even after just a few weeks. It all comes down to the retainer material you choose when fabricating retainers for your patients. Let’s look at why some retainer materials simply work better than others during your post-orthodontic care. The Difference The Right Retainer Material Can Make This is one of those things many dentists don’t really pause to think through during post-orthodontic care. At least not in the beginning. Usually, it comes up later, when a patient returns with slight shifting or a retainer that didn’t last as expected. And that’s when it starts making more sense. The material you choose isn’t just about “holding teeth in place.” It plays a much bigger role than that. In fact, the right choice can actually influence: How well the results last How comfortable the patient feels The frequency at which they need to come back for adjustments To sum up, retainer materials are worth paying attention to. Therefore, you need to check out the areas where a good retainer can actually help you. Here are some prove results: 1. It Helps Keep Teeth In Place For Longer. A good retainer material holds its shape and doesn’t lose its fit too quickly. If the material warps or softens over time, it stops doing its job properly, and that’s when teeth start to move again. 2. Patients Are More Likely To Actually Wear It. If a retainer feels bulky or looks obvious, patients tend to stop wearing it after a while. A material that’s comfortable and reasonably clear makes it easier for patients to stay consistent. And consistency is everything when it comes to retention. 3. Fewer Remakes And Fewer Return Visits. Retainers that break easily or stop fitting well bring patients back sooner than necessary. That costs time for both the patient and the practice. A more durable material from the start can reduce this quite a bit. 4. Less Chance Of Hygiene Problems. If the material you choose is highly perforated, it won’t help you at all. Most importantly, you will have a really tough time cleaning it. At the same time, if this continues for a long time, you will start to experience a foul odor and irritation or tingling in the gums. This means your post-orthodontic care has failed. As a result, you need a material with a finer texture and yet refined surface layering. The primary reason is that it will be easy to maintain. In addition, you will have fewer of the issues I discussed earlier. Why Not Every Retainer Material Behaves The Same If all retainer sheet materials worked the same way, choosing one would be simple. But they don’t, and the differences are more significant than they might seem at first. 1. Some are thicker and more rigid, others are thinner and more flexible. Rigid materials often provide stronger retention, but they can feel quite uncomfortable, especially for patients with smaller arches. Flexible materials are usually more comfortable but may not hold their corrective force as well over time. It’s a balance, and it shifts depending on the case. 2. Not all materials handle heat well. Some retainer materials can change shape slightly when exposed to warm temperatures, like hot drinks or a warm car. Even small distortions can affect how well the retainer fits. For patients who regularly drink tea or coffee, this is worth keeping in mind. 3. Clarity and staining vary between materials. Some materials go yellow or cloudy fairly quickly, particularly when patients consume coffee, tea, or other staining foods and drinks. For patients who care about how their retainer looks, that can affect whether they bother to wear it. Materials that remain clear longer tend to yield better results with these patients. 4. Some materials are easier to work with in the lab. Certain materials are more forgiving during the thermoforming process and give consistent results. Others need tighter controls to produce an accurate fit. If consistency in your lab workflow matters, this is worth factoring into your choice. How To Choose The Right Retainer Material If you ask me, there’s no one-size-fits-all answer here. Some patients are careful and follow instructions to the letter. However, others are still not so serious about that. For instance, you must have pain relievers after acidity regulators. But do you know which works better: omeprazole vs pantoprazole? Such knowledge gaps make small yet important differences in treatment. Meanwhile, that alone can change what will actually work long term. A material that looks great on paper might fail simply because the patient won’t wear it properly. You also have to think about their daily life. Are they always on the move? Do they tend to lose things? Are they likely to clean the retainer properly? These small details matter more than we usually admit. In practice, I’ve found it helps to talk to your lab as well. They often know which materials hold up better because they see what gets repaired or remade. Sometimes their feedback is more useful than any brochure or brand claim. Also, materials keep evolving. What was standard five years ago might not even be the best option today. So it’s worth staying a little curious and open to trying newer options when they make sense. At the end of it, you’re not just picking a material. To clarify, you are choosing what’s most likely to work for that specific patient sitting in front of you. Choose Better Post-Orthodontic Care Retainer materials don’t usually get much attention. People usually query about pain dampeners. For instance, tylenol vs ibuprofen, which is better? But it is time to discuss the real problems that poor retainer materials can cause throughout your post-orthodontic care. The choice you make here gradually affects everything. The factors that are most important in this connection are: Whether the patient actually wears it How stable are the results How often do they end up back in your chair for fixes? It’s easy to just go with what you’ve always used. Most of us do that at some point. But when you pause and think it through, case by case, you usually make better decisions. The best part is that fewer problems come up later. Disclaimer: This article is based on caregiving experience and is written for general awareness. It does not substitute for your doctor's advice. Always follow the treatment plan prescribed by your physician.
Whole CECT Abdomen Test: Cost, Uses, Procedure & Other Key Things You Should Know
Did your doctor just advice you to get the CECT abdomen test done? I am guessing you don’t yet know about this testis and why you need it. At the same time, many of us will also consider the cost of a test, which already sounds like a lot. At first, you need to know what a CECT abdomen? Why do doctors suggest this test? The last question that many sources don’t address is: Is an abdominal CECT worth your time and money? What Is A CECT Abdomen Test? In simple words, the acronym CECT means Contrast Enhanced Computed Tomography. To clarify, it is a CT scan of your abdomen. But how is this test different? During this test, lab experts inject a unique dye into the veins. Afer that, during imaging, the veins and organs are clearly visible. Imagine a neon object against the darkness. That’s how Contrast Enhanced Computed Tomography works. How Is It Different From Our Regular CT Scan? The CT scan can only provide a vague interpretation of the organs. However, the CECT abdomen highlights the specific areas. The illumination helps make it easy to understand what’s wrong with the belly! But how does the dye work? In simple words, the dye travels with your bloodstream. After that, it also illuminates the softer, smaller tissues. Let alone the organs. What Is The Purpose Of The CECT Abdomen Test? In most cases, doctors recommend this test to detect latent tumors. But that is not the only purpose. The dye is made from iodine and can travel throughout without causing harm. Therefore, it can also highlight issues like a liver abscess. Even if you are bleeding internally after an accident, you can still easily locate the bleeding. But the doctor does not always recommend a whole-abdomen CECT. If the problem is apparent but unclear, the doctor will suggest a CECT of the abdomen to evaluate the target organ. When Would A Doctor Ask For This Test? There can be a whole range of reasons. However, it is always impossible to apprehend why you need a CECT abdomen test. It depends on the suspects that the doctor is making: Unexplained Abdominal Pain Are you suffering from a dull and latent abdominal pain for months now? Oh, you did a USG, but it did not reveal anything? If the doctor suspects it is something more serious, like a hidden tumor, the go-to test is the CECT abdomen test. This test can also reveal whether you have a major infection that USG can’t spot. Or a chronic bleeding from a site. Suspected Cancer Or Tumor A USG tells you if you have a suspicious lump. However, it does not clarify whether it is a benign one or just a cyst. That’s where you need a test like a CECT of the abdomen. It can clearly differentiate what’s behind the tumor. Trauma And Accidents Often, we cannot realize internal hemorrhage after an accident. However, that may manifest in another form later. Therefore, you must rule out all chances of an internal injury through the CECT abdomen test. Kidney Stones And Urinary Issues In most cases, you can simply detect issues like a kidney stone with an ultrasound. However, problems like hydronephrosis are hard to detect. That’s where you need more effective tests, such as a CECT of the abdomen. CECT VS Plain CT Scan: What's The Real Difference? People often ask, "Doctor ne contrast scan kyun bola, plain se kaam nahi chalta?" Fair question. A plain CT scan works well for bones and can show gross structural issues. But when it comes to soft tissues of the liver, kidneys, intestines, or small blood vessels, it often misses subtle abnormalities. The contrast dye in a CECT dramatically enhances the visibility of these structures. For example, a 2 cm tumor in the liver might appear as normal tissue on a plain scan but stand out clearly after a contrast injection. Similarly, an early abscess or a small bleed in a blood vessel is far more reliably identified with contrast. That said, plain CT is sometimes preferred for patients allergic to contrast dye or with significant kidney disease, in which the dye could be harmful. Your radiologist will decide which one suits your situation. CECT VS MRI Abdomen: Which Is Better? This question comes up more often than you’d expect: CT scan or MRI, which one actually makes sense? Both give detailed images, yes. But they’re not substitutes for each other. A CECT scan is usually quicker. You’re in and out much faster compared to an MRI. It’s also easier to access, especially in smaller cities or diagnostic centers. That’s why in situations like accidents, internal bleeding, or suspected perforation, doctors don’t waste time. They go straight for a CT scan. Speed matters there. MRI is a different story. It’s slower, but more precise when it comes to soft tissues. So if the concern is something like a liver lesion, spine issue, or a pelvic condition, MRI tends to give more clarity. Another difference is that there is no radiation, which becomes important in cases like pregnancy or repeated scans. There’s also a practical side that people don’t always talk about. In many places, CT scans are simply more affordable than MRIs. So for urgent abdominal issues or even initial cancer checks, CECT often ends up being the first step. How Is The CECT Abdomen Procedure Done? It’s actually not as complicated as people imagine. When you arrive, they’ll usually ask you not to eat for a few hours beforehand. It is done to ensure that the scan comes out clearer. Someone at the desk or inside will also ask a few routine questions, mostly about allergies. If you’ve ever reacted badly to contrast dye or iodine, that’s something you really need to mention. In some cases, they might do a quick blood check. Not always, but it depends. Once that’s done, they’ll set up a small IV in your arm and have you lie down on the scanning table. The table moves slowly into the machine. When the contrast goes in, many people notice a sudden warm feeling, almost like heat spreading through the body. Some even say there’s a strange taste for a few seconds. It’s a bit odd the first time, but it passes quickly. During the scan, you’ll hear instructions to hold your breath for short bursts. That’s just to keep the images clear. The whole thing doesn’t take too long. Afterward, you’re free to go, as there is no real downtime. Just drink more water than usual for the rest of the day so your body can flush things out properly. CECT Abdomen Cost In India This is where it gets practical. The cost of a whole-abdomen CECT varies significantly depending on where you go. City / Setting Approximate Cost Range Government / CGHS / ESI hospitals ₹1,500 – ₹3,000 Tier-2 city diagnostic centers ₹2,500 – ₹5,000 Metro cities (Delhi, Mumbai, Kolkata, Chennai) ₹4,500 – ₹8,000 Premium corporate hospitals ₹7,000 – ₹12,000+ In eastern India, the charge for the CECT abdomen test is significantly lower. To clarify, you might have to pay something between ₹5,000 and ₹10,000. But are there any provisions for the people who cannot afford such costly tests? To clarify, the test is not the only medical procedure the patient is going through. The total cost might be unbearable for the patient's family. People who cannot afford the test can visit the CGHS-impaneled centers. Moreover, you can get the test done for free or at nominal charges at government medical college hospitals. But there is a loophole here. Often, the test price does not include the detailed radiologist’s report. So, ensure you get the test report at that cost as well. One Practical Tip: We often tend to pick the center that charges the least. Remember, the quality of the CT scan machine matters a lot here. To clarify, the 64 slice machines don’t perform as well as the 128 slice machines do. At the same time, the radiologist's efficiency in performing the test matters. Risks And Side Effects That Every Suspect Must Know CECT is very safe for most people. But like any medical procedure, it carries some considerations. Radiation Exposure CT scans use X-ray radiation, more than a plain X-ray. A single CECT abdomen delivers roughly 10–15 mSv of radiation. That's not trivial if you're having scans repeatedly. Your doctor should recommend it only when medically necessary. Contrast Reactions After the test, the mild reactions include nausea, itching, or a rash, which typically resolve on their own. At the same time, severe allergic reactions (anaphylaxis) are rare but possible. But don’t worry, as all centers can tackle such minor developments. Kidney Risk The kidneys filter the contrast dye. In patients with pre-existing kidney dysfunction, it can very rarely cause contrast-induced nephropathy. As a result, you need to have a creatinine level checked before the scan. This step largely prevents this risk. Not Suitable For Pregnancy Radiation exposure during pregnancy is not a good call. Therefore, doctors try to avoid it when you are pregnant. However, they can suggest a test in a very serious situation. Should You Be Worried About Going For This Test? If the doctor has asked you to have a CECT abdomen, you must go for it. Do not delay or avoid it at any cost. However, the main concern is whether there is some obvious risk if the doctor suggests it? Across India, doctors suggest thousands of CECT abdomen tests every day. So you should not start worrying! In addition, the whole test goes painless. At the same time, it is quick and helps the doctor to study the whole abdominal anatomy. The dye is usually harmless. So there is no great risk involved. But ask your doctor about the preparations that you need to take before proceeding with the test. Disclaimer: The purpose of this content is to make the readers aware and cautious about health concerns. Do not takeany advise shared or health trend discussed in this piece as obvious and always hold. Before making any medical call, always consult a trained and licensed doctor in the field. If you need any other health tips or want to hear health-related recovery of diagnosis cases, visit worldhealthlife.com.
What Foods Produce Sperm Fast? A Complete Beginner Friendly Guide
Eggs, walnuts, spinach, pumpkin seeds, bananas, dark chocolate, garlic, tomatoes, pomegranate, and ashwagandha. Meanwhile, there are some common foods that deplete sperm count snd quality also! My friend Rico found out he had a low sperm count of 34. But he was a quite healthy guy. Usually, he plays basketball on weekends, doesn't smoke, and is not overweight. So, I really did not expect to hear that from him. His doctor asked him what he eats on a regular day. Rico thought about it. His staple is rice every meal, processed meat for breakfast most days, chips in the afternoon, and beer on weekends. I know that ddoesn’t sound healthy. However we can call that normal. However things do not always play out as we expect. Sperm quality doesn't depend on your food practices after all. On the contrary, it depends on what you particularly eat! Again, that brings us to the question: what foods produce sperm fast. Why What You Eat Directly Affects Sperm Production? Your body makes sperm every single day. The actual rate is around 1,500 per second. So what is the role of the nutrition that you draw from the food there? Your food habits directly impact sperm quality. In addition, they improve the sperm count and the sperm shape as well. The healthy sperms move fast too. So, that’s how good nutrition elevates sperm’s overall quality. But it is not actually the food. Instead, the sperm needs a bunch of micro and macro nutrients specifically: The Key Nutrients Essential For Better Sperm Health Zinc, helps in testosterone production and sperm count Folate (B9), is best for sperm shape and chromosomal health Vitamin C protects sperm from oxidative damage Vitamin E looks after overall sperm quality Omega-3 fatty acids sharply improves sperm motility (how well it swims) Selenium enhances sperm development Coenzyme Q10 stores cellular energy for sperm Most Filipino men are low in zinc and folate without knowing it. Again, you won’t face any drastic symptoms if you lack them. That’s why most Filipino men remain unaware. However, the sperm’s utility and quality degrade slowly. What to do: Before spending money on supplements, fix the food first. Supplements can surely help here. However, you cannot deny the role that nutrients available from food play. What Foods Produce Sperm Fast: The Complete Breakdown If you are a Filipino with low sperm count, here are some foods you cannot keep away from your diet: 1. Eggs Two eggs a day is probably the easiest thing on this list. They're high in protein and Vitamin E, and they're cheap. Most importantly, you can get eggs anywhere and work with every meal. Vitamin E specifically protects sperm cells from damage during development. Most men don't get enough of it. But eggs are one of the simplest fixes. Quick fix: Drop the hot dog from your breakfast. Add two eggs instead. 2. Walnuts Rico started eating walnuts. The doctor suggested that he just take a small handful every morning. About two months in, his numbers had improved. His doctor said it wasn't just the walnuts. Certainly, he changed a few things. But walnuts were the one thing he was consistent about, the whole time. They contain omega-3 fatty acids that directly support sperm count and movement. However doctors say that unsalted walnuts are always better. A small bag from the grocery is enough for weeks. What to do: Keep walnuts somewhere visible. It can be on your desk, in your bag, or on the kitchen counter. If you have to hunt for them, you won't eat them. 3. Spinach I know spinach are boring. But folate deficiency is one of the most common and overlooked causes of poor sperm quality. Again, spinach is one of the easiest sources of it. Low folate = poorly shaped sperm, and a higher risk of chromosomal problems. But the good news is you don't need to eat salads. What you can do is simply throw spinach into sinigang. Or add it to fried rice. I prefer to have it with soup. It takes on the flavor of whatever it's cooked with. Quick fix: Tonight, add one handful of spinach to dinner. That's the whole task. But avoid that if you have uric acid symptoms. 4. Bananas This is a cheap option. Best of all, bananas are available at every palengke and sari-sari store. If you spermm count is low, you cannot ignore bananas by any means. Bananas contain bromelain. That’s an enzyme involved in regulating sex hormones. At the same time, you get B1 and Vitamin C for sperm energy and motility. Lastly, having bananas is the easiest meal habit for anyone. Just have one banana in the morning. It takes ten seconds with no prep. What to do: Eat one before breakfast. Again, make it a daily habit! 5. Pumpkin Seeds This is a solution that is not often discussed. Pumpkin seeds are among the best food sources of zinc you can eat. At the same time, zinc is arguably the most important mineral for male fertility. When you lack zinc, the testosterone level drops fast. At the same time, you suffer from low sperm development. In Philipines, men suffer from zinc deficiency. However, a lot of them don’t realize that. But do you know how to get seeds? In most shops and markets, you will get seeds in packaged format. Quick fix: Mix pumpkin seeds with your walnuts. That’s how you can combine the benefits of two sperm-vitalizing foods. 6. Dark Chocolate Do you know dark chocolate is important for managing your sperm health? But milk chocolate is not good for, or even necessary for, sperm health. But why do dark chocolates help? Firstly, dark chocolates give you L-arginine, which is an amino acid needed fpr better sperm count. It also makes spers faster. 7. Garlic Garlic has allicin, which improves blood flow to reproductive organs. It also contains selenium, which plays a direct role in sperm development. It's already in almost every Filipino dish. You just need to be less stingy with it. What to do: Double the garlic in whatever you're cooking. So, that’s the easiest upgrade on this list. But stop the overdose if you have a right upper quadrant pain. 8. Tomatoes Tomatoes are high in lycopene. It is an antioxidant that multiple studies have linked to better sperm count, motility, and structure. It's one of the better-researched nutrients for male fertility. But tomatoes are already a proper part of Filipino cooking. For example, you need tomatoes to prepare sinigang, sawsawan, and most of the stews. Just make sure they're actually in your meals and not just garnish. 9. Pomegranate No doubt pomegranates are harder to find regularly in Philipines. However, they must pick them up when you see them. Remember, pomegranate fights oxidative stress. Again, that is one of the main things quietly damaging sperm quality over time. But a lot of people can’t find fresh pomegranate in Philipines. Therefore, they can add 100% pomegranate juice in their diet with no added sugar. Even a small glass a few times a week helps a lot. 10. Ashwagandha Yes it is a supplement. However, it is one of the best natural supplements that is as essential as these diet forms. Again, ashwagandha is easy to find. Go to any drug store. Or fotness and welllness stores. They always have it in powder and capsule forms. A lot of studies show that ashwagandha can directly improve male fertility. More importantly, it can improve testosterone. However, the best part is that it can enhance the sperm count besides improvimg motility among males. However we cannot ignore the fact that it is a supplement. So before you start having additional ashwagandha, consult your doctor. Bonus Tip: When you are having these foods on a daily basis, that is the best time to take creatine for muscle gain too. Foods That Are Working Against You Right Now Now you know what foods produce sperm fast. However, you also need to know which foods can deplete sperm count and quality. What’s most important, these foods are there in our daily list too: Processed meats in hot dogs, longganisa, and tocino. Preservatives in these can reduce sperm quality. However, doctors don’t ask you to stop eating processed meat. Just don’t make it a regular practice. Too much sugar disrupts hormone levels. So you need to quit the soft drinks, especially. Trans fats, like those in most fried street food and packaged snacks, are also harmful to sperm count and quality. Trans fats are directly tied to lower sperm count in research. Alcohol is also an important name in the list. More than a few drinks a week reduces testosterone and sperm production. Weekend sessions also add up. Excessive caffeine is harmful to you. However, one coffee is fine. Three energy drinks are not. Plastic food containers with BPA are also harmful. However, most of our packaged foods come in that. So that's another habit we need to get rid of fast. The intention of this article is to offer general advice based on research. We don’t intend to provide genuine medical guidance. For authentic medical guidance contact a licensed doctor in Philipines. All foods suggested are based on authentic medicinal research. However, people with hyperspermia should strictly avoid these foods.
Early Pregnancy Discharge: What It Actually Looks Like And When to Worry?
Have you recently just found out you might be pregnant? Or waiting for the final report from the doctor anxiously? Meanwhile, you can easily diagnose a lot of important things. At first, consider whether you have pain. It might not be a prominent one, but damp and dull. Often, you feel weird cramps in your abdomen, too. Try to act on these signals quickly. So is everything normal? Or do these signs mean you should call the doctor immediately? Relax. Don't panic, there is nothing wrong with you. Increased discharge is a common sign of early pregnancy. Doctors call it the early pregnancy discharge. On the contrary, it is a good sign that makes you aware of your pregnancy much early. What more can an early pregnancy discharge tell you? What Is Vaginal Discharge? The body produces a fluid by default. When fluid leaves the body through the vaginal tract, it is called vaginal discharge. But contrary to what many people assume, it is not an indicator of Something wrong with the body. Often, we see early pregnancy discharge when the cervix produces mucus during your cycle. However, that is a clear indicator of hormonal change. Whether it's ovulation, before the menstrual cycle hits, or during early pregnancy, hormonal discharge can cause vaginal discharge. Healthy VS. Unhealthy Discharge: How To Tell The Difference Normal, healthy discharge is: Thin in texture Clear or milky white in color Mild in smell or has no smell at all That's it. There are rarely more variations than that. What to do: If your discharge matches that description, you're most likely fine. Unhealthy discharge looks different. Therefore, you need to watch out if yours is: Foul-smelling Green or yellow Chunky or cottage-cheese-like Accompanied by itching, burning, or pain when you pee Quick fix: Any of those signs means you need to take the doctor's advice. Don't Google yourself into a spiral. Act as your doctor says! To maintain health during this stage, follow the 1 to 3 month pregnancy diet chart. Early Pregnancy Discharge: What's Actually Happening? In a sample study, a patient said this about early pregnancy discharge: "I kept thinking I was getting my period. There was more moisture than I'd ever noticed before. But it was clear and didn't smell like anything. I was four weeks pregnant and had no idea." This is how many women actually discover what is happening to them. So now let's address the question: what causes the early pregnancy discharge? According to the NHS, early pregnancy discharge is associated with a high degree of protection. The heavier fluid flow indicates a barrier that prevents infections from ascending into the urethral chamber. What Does It Actually Look Like? If it is the healthy kind of early pregnancy discharge, it goes by the name of leukorrhea. It's the same type of discharge you may have noticed before. In simpler words, it usually looks: Thin and watery or slightly sticky Clear to milky white Mild or odorless What To Do? The discharge volume is the key here. For instance, if the discharge is clear and has no unpleasant odor, it means your body is in good condition. That's the first prenatal observation you should not miss. Again, if this continues during the first trimester, consult your doctor. Meanwhile, get the fetal heart rate checked as well. Other Things That Can Change Your Discharge Your discharge volume and quality depend on many other things. For example, multiple factors can alter how your discharge smells and feels in your hand. Remember, there are plenty of horizontal changes and quick alterations that you cannot miss. As a result, you need to know why you see what you see: What You See What It Might Mean Thick, chunky, cottage cheese texture Yeast infection (thrush), which is very common in pregnancy Fishy smell, thin and grayish Bacterial vaginosis Yellow or green, possibly frothy Trichomoniasis (a common STI) Yellow or green with pelvic pain or bleeding Possible chlamydia or gonorrhea Discharge from blisters or sores Could indicate genital herpes During pregnancy, many women suffer from yeast infections. But why does yeast grow? The internal environment is favorable for yeast growth due to the hormonal balance at this stage. Other Early Signs of Pregnancy Discharge by itself doesn’t really confirm anything. People often look for one clear sign, but pregnancy rarely works like that. It’s usually a mix of small changes that start showing up together. Some of the early things people notice are pretty familiar: A missed period (this is the one most people pick up on first) Breasts feeling sore or slightly heavier than usual That wave of nausea, especially in the morning, though not always Suddenly wanting certain foods or suddenly undergoing an appetite loss, where even the smell puts you off Feeling tired in a way that’s hard to explain Going to the bathroom more often than you normally would Random headaches here and there Mood swings that don’t quite match the situation A bit of bloating or light cramping However, I must clarify that a single missed period does not conclusively tell that you are pregnant. Again, there are several reasons that can lead you to miss a period: Feeling stressed Fluctuations of body weight Taking birth control pills Any of the issues can set off a temporary surge in the body. As a result, the body caps in the outflow. In the same vein, many people prefer to take a home pregnancy test. That’s a private way to understand what you're going through. What to do: There will be at least some clearly visible signs when you are pregnant. The bet partis that most of these signs will always show up together. As a result, when they appear, you will know that it is the case of early pregnancy. When Should You Actually Call A Doctor? Most people actually delay calling a doctor. But please do not make the same mistake. The early pregnancy discharge gives you obvious signs that you are pregnant. However, you still need a doctor to verify it. In addition, you can confirm a pregnancy with a home test. However, you need a doctor to make the final call. In this connection, you must also know when you should actually start worrying and go see a doctor rather soon: Your discharge has a strong or unusual smell There's itching, burning, or pain alongside it You see any blood that doesn't match a normal period, this can sometimes be implantation bleeding. But it can also signal something that needs attention) When Something just feels "off" trust that instinct The Short Version Your early pregnancy discharge should be less dense, clear, and preferably white. At the same time, it should not smell foul. But I hope you now understand why it happens. Simply put, it happens due to the rise in estrogen. Therefore, the body starts working in a fight-or-flight response. Its main goal is to protect pregnancy. Can you relate to what you have read so far? Then it is nothing serious. But you should start worrying when the discharge looks yellowish or starts to smell bad. For instance, when the discharge is greenish or seems chunky, that is a very bad signal. In that condition, your prime goal should be to see a doctor as soon as possible. Each of these cases indicates you are experiencing a serious condition. The doctor will verify what it is and how serious it is. Disclaimer: This article is only meant for sharing information. It offers no actual medical help. If you are facing genuine health concerns tt is always better to see a doctor first.