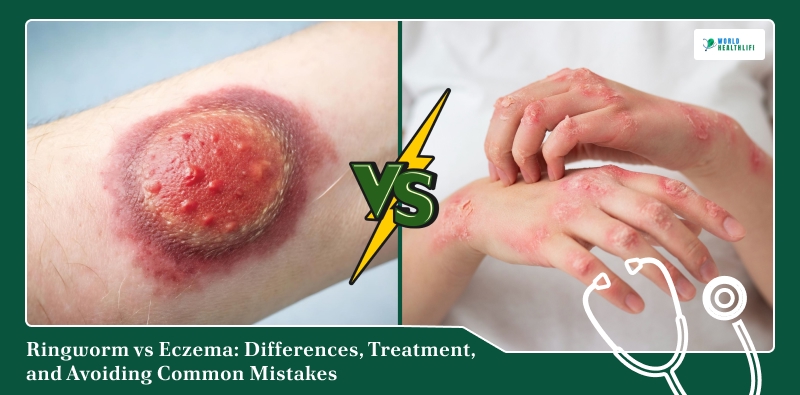
Skin rashes have a way of making simple things feel uncertain. For instance, a patch might show up. It might be red, itchy, or dry in an unnatural circular way. Suddenly, the internet is suggesting five different explanations. This is where people get confused about ringworm vs eczema.
To be honest, both can itch, scale, and linger for a long time. However, if you ignore the similarities, they actually belong to very different clinical categories. Also, any treatment that helps one might quietly aggravate the other.
In fact, many people make the same mistake early on. They treat the appearance and ignore the mechanism. That is where trouble starts. Although they look similar, they have different biology, risks, and treatment.
Ringworm vs Eczema: Why Do People Mix Them Up
It is understandable why people get confused about ringworm vs eczema. In real life, skin disease rarely presents like textbook photography.
Ringworm does not always open with a neat circular ring. Meanwhile, eczema does not always remain confined to the classic flexural creases. This holds when chronic scratching, dryness, or secondary irritation is present.
Moreover, early lesions can look unfinished, almost vague. Just a patch, a rough border, a little redness. It is enough to blur the line if the rash is being judged quickly, or worse, treated quickly.
The bigger problem is that people often chase relief before diagnosis. They reach for whatever cream is already in the cabinet. Hydrocortisone, antifungal, moisturizer, some herbal product, some random internet recommendation. Some of those choices are harmless detours. Some are not.
In addition, steroid application for an undiagnosed fungal rash suppresses visible inflammation. It might be just enough to obscure the lesion while the infection continues beneath it. That creates a worse picture and a slower recovery.
Understanding Ringworms
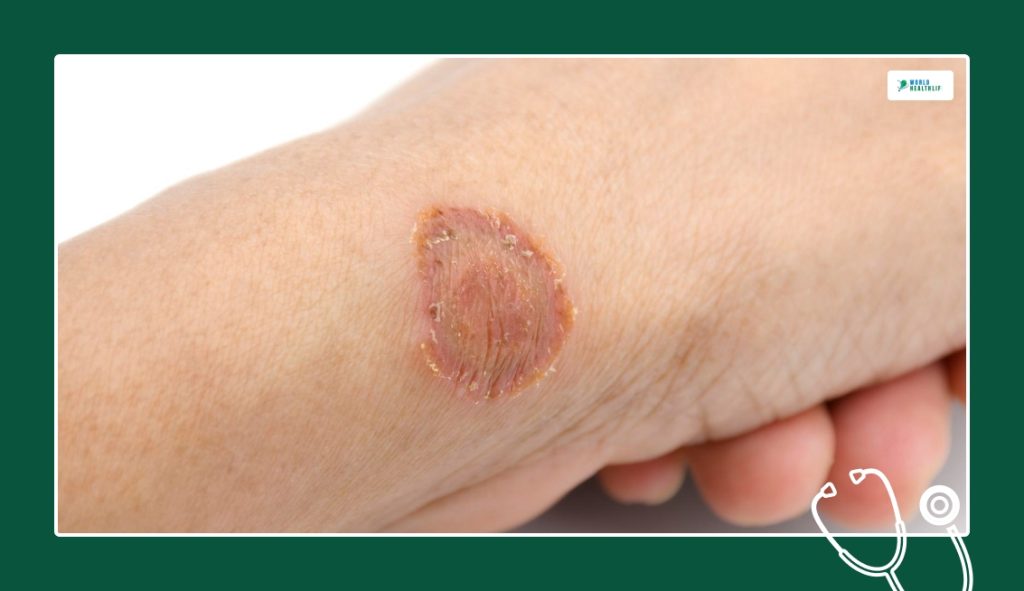
Ringworm, or tinea corporis, is a superficial dermatophyte infection of the skin. However, it is not caused by a worm. That old name stuck because the rash mostly forms a ring-like configuration with an advancing border.
Basically, the organism feeds on keratinized tissue. This means skin, hair, and nails all become targets depending on the location. Moreover, the factors that facilitate fungal transmission include warmth, friction, moisture, shared surfaces, and close contact.
Clinically, the lesion tends to expand from the outside. At the outset, the outer border is the most active. So there may be more scale, redness, or elevation there. Meanwhile, the center looks calmer or partially cleared.
Moreover, mild to moderate itching is common. Burning is less classic. Also, the naming changes if the scalp, nails, feet, or groin are involved. However, the fungal logic remains the same.
Typical Ringworm Clues
Some signs tend to lean towards fungal rather than inflammatory. This happens especially when they appear together. The following are some clues:
- A circular or oval patch with a clearer center
- The edge is raised and scaly. Also, it slowly spreads outward
- A history of contact with pets, locker rooms, shared towels, or infected family members
However, the pattern might be persuasive. This happens when the lesion behaves as if it is moving outward rather than simply flaring in place.
Understanding Eczema
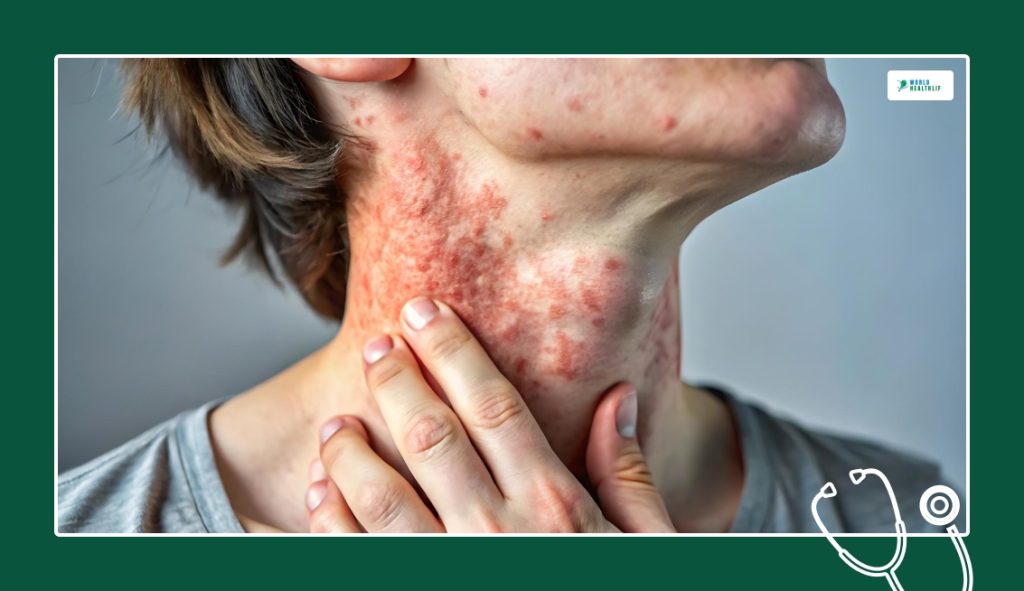
Unlike what most people think, eczema is not a single skin condition. In everyday use, it might mean atopic dermatitis or a broader eczema pattern. The latter is marked by impaired barrier function, chronic dryness, inflammation, and recurrent itch.
This is where the skin loses its ability to retain moisture and defend itself effectively. Also, it is more reactive to irritants, allergens, friction, stress, climate change, and scratching. That cycle can repeat for years.
This is why eczema often feels inconsistent. It can improve, then flare. It can look angry in winter, then settle with humidity and routine care, then return after stress, detergent exposure, or sleep disruption.
The shape is often less disciplined than that of ringworm. Borders are fuzzier. Texture matters more. Cracking, lichenification, dry, rough skin, and itch that becomes compulsive are strong clues.
Actually, the lesion is not spreading because of fungal growth. Rather, it is evolving because the skin barrier is failing. Meanwhile, the immune response keeps feeding the irritation.
Common Eczema Clues
In general, people with eczema show a broader context around the rash rather than just the rash itself. The following are some of the major patterns:
- A personal or family history of allergies, asthma, or sensitive skin
- Flare patterns linked to soaps, fabrics, weather shifts, or stress
- Repeated itching that thickens the skin over time
That broader history often distinguishes eczema from look-alike conditions. Not instantly, but eventually, yes.
How to Differentiate: Ringworm vs Eczema
If ringworm vs eczema is compared in a clinical setting, the most useful question is not “Which one looks redder?” It is “How is this lesion behaving?” Ringworm tends to declare itself through border activity. The edge becomes the most noticeable part.
In general, eczema tends to present with texture, itch burden, recurrence, and context. Moreover, in many cases, it behaves like a chronic inflammatory skin problem.
Although location helps, it must never be the sole factor. For instance, eczema tends to affect flexural areas. These include
- Insides of the elbows
- Behind the knees
- Wrists
- Hands
- Neck
Meanwhile, ringworm can appear almost anywhere, including places where eczema is less classically centered. Contagiousness also matters. Eczema does not pass from one person to another. However, ringworm absolutely can.
If multiple household members have suspicious patches, fungal transmission deserves real consideration.
Comparison Chart: Key Differences At A Glance
| Feature | Ringworm | Eczema |
|---|---|---|
| Root cause | Fungal infection | Inflammatory skin disorder |
| Contagious | Yes | No |
| Border | Often raised and defined | Often diffuse or irregular |
| Center of lesion | May look clearer | Usually no central clearing |
| Itch pattern | Mild to moderate | Often intense and persistent |
| Common strategy | Antifungal therapy | Barrier repair and anti-inflammatory care |
This chart helps, but only up to a point. Skin does not always follow neat columns. Some eczema patches are round, while others are subtle. In the end, the right diagnosis still depends on looking at the whole picture rather than a single visual clue.
Wrong Treatment Creates Bigger Problems
Ringworm vs eczema is not merely an academic distinction. In fact, the wrong treatment becomes a practical mistake with consequences.
For instance, if a fungal infection is treated like eczema, especially with topical steroids, there are consequences.
In this case, the redness may fade before the fungus is actually controlled. That creates a modified appearance sometimes called tinea incognito. The rash becomes less obvious and more stubborn. It has not improved in the real sense. It has been disguised.
The reverse error is less dangerous but still unhelpful. If antifungal creams are applied to eczema, the skin usually stays inflamed because the driver was never fungal to begin with. Some patients then assume the rash is “resistant” when, in fact, it was just misidentified.
Meanwhile, the barrier keeps deteriorating. It includes more scratching, dryness, and inflammation. The clock keeps running while the skin gets less cooperative. This is how common rashes become prolonged ones.
What Treatment Works Best?
When it comes to treating ringworm and eczema, the approaches and treatments differ. This is because the two conditions differ markedly at the clinical level.
1. Managing Ringworms
At the outset, localized ringworm responds well to topical antifungal agents. However, it must be used consistently for the full treatment window, not just until the rash looks better.
In fact, stopping too soon is one reason fungal lesions recur. Also, it is important to keep the skin dry where possible. Moreover, contaminated items such as towels, sports gear, hats, or bedding may require attention depending on the site involved.
Meanwhile, scalp or extensive disease mostly requires oral therapy rather than creams alone.
2. Managing Eczema
Eczema treatment is less about killing a culprit and more about rebuilding control. Regular emollients restore barrier function. Trigger reduction lowers reactivity. Short courses of anti-inflammatory medication may calm active flares.
In recurrent disease, maintenance strategy matters as much as rescue therapy. Patients usually do better when their own pattern is understood.
- Which soap causes trouble?
- Which weather shift changes everything?
- What are the areas that flare first?
Good eczema management is not random. Rather, it is repetitive, disciplined, and often a bit boring. That is why it works.
Stop Doing Self-Diagnosis Now!
There are situations when guessing does not help at all. For instance, the following cases deserve proper evaluation if a rash is:
- Spreading
- Recurring
- Becoming painful
- Involving the scalp or nails
- Failing to improve after a reasonable first attempt at treatment.
The same is true if the lesion is oddly shaped or secondarily infected. The same is true if it shows mixed features that do not fit cleanly into a single category.
In general, dermatology is full of imitators. Psoriasis, pityriasis rosea, contact dermatitis, nummular eczema, seborrheic patterns, and fungal overlap.
This is also the point at which ringworm vs eczema should be treated as a diagnostic framework rather than a final answer. Also, clinicians may use exam findings alone. Or, they might add skin scraping, fungal microscopy, or culture when the appearance is uncertain.
The goal is not overtesting. Rather, it is about breaking the cycle of trial and error and partial treatment that keeps people inflamed for weeks longer than necessary.
Frequently Asked Questions (FAQs)
Yes. In fact, some eczema patches are round and scaly. This might cause visual confusion.
No. Early lesions may appear incomplete or irregular before the classic border forms.
Yes, it does. Also, it may reduce redness while allowing the fungal infection to spread beneath the skin.
No. In fact, eczema does not spread from person to person.
It is time to see a dermatologist if the rash spreads, recurs, causes pain, or does not improve after initial treatment.
The Right Diagnosis Changes Everything
Most rash mistakes happen because the eye sees similarity and the mind assumes sameness. That assumption fails here. Ringworm vs eczema may look like a small distinction on day one, but it can change the entire treatment path. However, fungal disease needs eradication.
Meanwhile, eczema needs barrier restoration and inflammation control. If you understand that split, there will be no confusion. In fact, not every itchy patch needs urgency, but every persistent one deserves accuracy.